More to explore
-
 Local News 4/24/24Man charged in Tuesday apartment shooting in Cape Girardeau1A man is facing three felony charges in connection with a Tuesday, April 23, shooting that left one person wounded. Cape Girardeau County Circuit Court documents indicate Prosecuting Attorney Mark Welker has charged Michael Dewayne Thompkins with...
Local News 4/24/24Man charged in Tuesday apartment shooting in Cape Girardeau1A man is facing three felony charges in connection with a Tuesday, April 23, shooting that left one person wounded. Cape Girardeau County Circuit Court documents indicate Prosecuting Attorney Mark Welker has charged Michael Dewayne Thompkins with... -
 Local News 4/24/24Cape Girardeau school board to implement cellphone pouches at junior high, buy out leased pouches at high school6The Cape Girardeau School District Board of Education voted unanimously Monday night to implement the YONDR cellphone pouches at Terry W. Kitchen Central Junior High School for the 2024-25 school year, in addition to buying out the current stock of...
Local News 4/24/24Cape Girardeau school board to implement cellphone pouches at junior high, buy out leased pouches at high school6The Cape Girardeau School District Board of Education voted unanimously Monday night to implement the YONDR cellphone pouches at Terry W. Kitchen Central Junior High School for the 2024-25 school year, in addition to buying out the current stock of... -

-

-

-

-

-

-

-
 Local News 4/23/24Cape man pleads guilty to 15-year-old's 2019 murder3A Cape Girardeau man pleaded guilty Monday, April 22, to the 2019 killing of a 15-year-old girl. A release from Cape Girardeau County Prosecuting Attorney Mark Welker says Isaiah Lane, 33, pleaded guilty in circuit court to second-degree murder and...
Local News 4/23/24Cape man pleads guilty to 15-year-old's 2019 murder3A Cape Girardeau man pleaded guilty Monday, April 22, to the 2019 killing of a 15-year-old girl. A release from Cape Girardeau County Prosecuting Attorney Mark Welker says Isaiah Lane, 33, pleaded guilty in circuit court to second-degree murder and... -

-
 Local News 4/23/24Jackson teacher, coach receives national speech, debate, theater educator awardJackson High School speech teacher Bob Clubbs was honored over the weekend with an award from the National Federation of State High School Associations. During the Missouri State High School Activities Association state speech, debate and theater...
Local News 4/23/24Jackson teacher, coach receives national speech, debate, theater educator awardJackson High School speech teacher Bob Clubbs was honored over the weekend with an award from the National Federation of State High School Associations. During the Missouri State High School Activities Association state speech, debate and theater... -
 Local News 4/23/24Show Me Strong Kids Regional ECHO Program to hold virtual meetings sessionsThe Show Me Strong Kids Regional ECHO Program will host virtual meeting sessions over Zoom for local child-serving professionals starting Tuesday, April 30. ECHO stands for Extension for Community Healthcare Outcomes and uses teleconference sessions...
Local News 4/23/24Show Me Strong Kids Regional ECHO Program to hold virtual meetings sessionsThe Show Me Strong Kids Regional ECHO Program will host virtual meeting sessions over Zoom for local child-serving professionals starting Tuesday, April 30. ECHO stands for Extension for Community Healthcare Outcomes and uses teleconference sessions... -

-
 Local News 4/23/24Connection Point Church to host 'Conquering the Beast Men’s Event'3Connection Point Church will host its “Conquering the Beast Men’s Event” on Saturday, May 4. The event, at 358 E. Deerwood Drive in Jackson, will feature guest speaker Scott Mendes, who is a professional bull-riding champion. According to a news...
Local News 4/23/24Connection Point Church to host 'Conquering the Beast Men’s Event'3Connection Point Church will host its “Conquering the Beast Men’s Event” on Saturday, May 4. The event, at 358 E. Deerwood Drive in Jackson, will feature guest speaker Scott Mendes, who is a professional bull-riding champion. According to a news... -
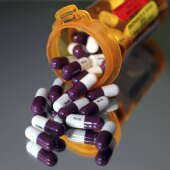 Local News 4/23/24National Drug Take Back Day is Saturday, but drug disposal is ‘year-round need’While the United States Drug Enforcement Agency’s annual National Prescription Drug Take Back Day is coming up on Saturday, April 27, medicine disposal is considered a "year-round need." According to a news release from the Pharmaceutical Product...
Local News 4/23/24National Drug Take Back Day is Saturday, but drug disposal is ‘year-round need’While the United States Drug Enforcement Agency’s annual National Prescription Drug Take Back Day is coming up on Saturday, April 27, medicine disposal is considered a "year-round need." According to a news release from the Pharmaceutical Product... -

-
 Local News 4/22/24Death investigation underway in Scott CountyBENTON — A death investigation is underway in Scott County. Scott County Sheriff Wes Drury confirmed one person is custody following an incident early Monday, April 22 in rural Scott County. Further information will be available later Monday, the...
Local News 4/22/24Death investigation underway in Scott CountyBENTON — A death investigation is underway in Scott County. Scott County Sheriff Wes Drury confirmed one person is custody following an incident early Monday, April 22 in rural Scott County. Further information will be available later Monday, the... -
 Local News 4/22/24Community Counseling Center Foundation wants communities to ‘go green’ for Mental Health Awareness Month1For Mental Health Awareness Month in May, the Community Counseling Center Foundation hopes to see as many towns lit up with the color green as possible across the five counties the center serves. Mental Health Awareness Month was established in 1949...
Local News 4/22/24Community Counseling Center Foundation wants communities to ‘go green’ for Mental Health Awareness Month1For Mental Health Awareness Month in May, the Community Counseling Center Foundation hopes to see as many towns lit up with the color green as possible across the five counties the center serves. Mental Health Awareness Month was established in 1949... -
 Local News 4/22/24Zonta Club to hold ‘Men of Courage’ event to raise sexual-assault awarenessZonta Club of Cape Girardeau will host a breakfast event Monday, May 6, that is open to all men and promotes unity toward efforts to end sexual assault and violence. The event, titled "Men of Courage: Together We End Sexual Assault", is the first...
Local News 4/22/24Zonta Club to hold ‘Men of Courage’ event to raise sexual-assault awarenessZonta Club of Cape Girardeau will host a breakfast event Monday, May 6, that is open to all men and promotes unity toward efforts to end sexual assault and violence. The event, titled "Men of Courage: Together We End Sexual Assault", is the first... -

-

-

-

-
-

-
 Photo Gallery 4/20/24Chaffee Prom 2024
Photo Gallery 4/20/24Chaffee Prom 2024 -

-
 Most read 4/19/24Inside Becca’s Closet: A mission to dress teens for formal events2The organization Becca’s Closet, which helps young girls get access to formal dresses for dances and proms, is celebrating its 20th anniversary this year. Cape Girardeau is the home to one of two Missouri chapters, and one of 51 in the U.S...
Most read 4/19/24Inside Becca’s Closet: A mission to dress teens for formal events2The organization Becca’s Closet, which helps young girls get access to formal dresses for dances and proms, is celebrating its 20th anniversary this year. Cape Girardeau is the home to one of two Missouri chapters, and one of 51 in the U.S... -
 Most read 4/18/24Tenmile looks to add balcony to old Esquire Theater building2Cape Girardeau City Council approved a license and indemnity agreement with Tenmile Holdings LLC on Monday, April 15, for the installation of a marquee sign and awning with column posts for the old Esquire Theater building. ...
Most read 4/18/24Tenmile looks to add balcony to old Esquire Theater building2Cape Girardeau City Council approved a license and indemnity agreement with Tenmile Holdings LLC on Monday, April 15, for the installation of a marquee sign and awning with column posts for the old Esquire Theater building. ... -
 Most read 4/18/24Police: Bollinger County woman told elaborate lies across multiple investigations, including sexual assault5BOLLINGER COUNTY — Police say a Bollinger County woman told several elaborate lies during sexual assault and harassment investigations in a complex and escalating scheme that targeted the mother of her fiance’s child. Michelle D. Kaempfer of Glen...
Most read 4/18/24Police: Bollinger County woman told elaborate lies across multiple investigations, including sexual assault5BOLLINGER COUNTY — Police say a Bollinger County woman told several elaborate lies during sexual assault and harassment investigations in a complex and escalating scheme that targeted the mother of her fiance’s child. Michelle D. Kaempfer of Glen... -
 Most read 4/18/24City Tavern: Belly up to the bar after Sunday serviceJust when I thought I’d run out of new restaurants to try, a friend with good judgment suggested I might want to take a quick road trip over to City Tavern in downtown Perryville for some good old homestyle cooking. I was intrigued by the...
Most read 4/18/24City Tavern: Belly up to the bar after Sunday serviceJust when I thought I’d run out of new restaurants to try, a friend with good judgment suggested I might want to take a quick road trip over to City Tavern in downtown Perryville for some good old homestyle cooking. I was intrigued by the... -

-